
April Donovan host our Hospice Page and is a Senior Advocate for Michigan Judicial Probate Integrity Project.
WELCOME TO MICHIGAN’S HOSPICE SPOTLIGHT!

My name is April Donovan and my mother, Twila J. Apger, was a victim of guardianship abuse by a family member, nursing home abuse/neglect, and her death was hastened by hospice. If you’re interested in learning more about my mom’s case and my fight for justice for her, you can join the Facebook group - JUSTICE for TWILA APGER. I’m also on multiple social media platforms - @justicefortwila.
On this section of the Michigan Judicial Probate Integrity Project’s website, I will be shedding light on what happens inside some of these hospices we have here in Michigan. If you have any questions, please feel free to contact me! You are not alone in feeling like you are being lied to and your loved one is ultimately being murdered.
“Comfort” Kit:
Fentanyl Patch (Transdermal)

Commonly used Hospice drugs:
*Pain Management: Morphine (Roxanol), Hydrocodone, Dilaudid, Methadone, and Acetaminophen (suppository).
*Anxiety/Restlessness: Lorazepam (Ativan), Haloperidol (Haldol), Quetiapine, and Thorazine.
*Nausea/Vomiting: Haloperidol, Prochlorperazine (Compazine), Promethazine (Phenergan), and Reglan.
*Respiratory Distress/Excess Secretions: Atropine (drops), Hyoscyamine (Levsin), and Morphine.
*Constipation/Other: Bisacodyl (Dulcolax) and other stool softeners. Benadryl.
***RISKS***
Mixing benzodiazepines (Ativan) with opioids (Morphine) or antipsychotics (Haldol) causes falls, confusion, respiratory depression, coma/sedation, and death especially in older adults.
FENTANYL PATCH (TRANSDERMAL)
Fentanyl skin patch is used to treat severe pain. Fentanyl is a strong opioid analgesic (pain medicine). It acts on the central nervous system (CNS) to relieve pain.
Elderly patients are more likely to have drowsiness and age-related lung, kidney, liver, or heart problems, which may require caution and an adjustment in the dose for patients receiving fentanyl skin patch.
The presence of other medical problems may affect the use of this medicine, like:
Addison's disease (adrenal problem) or
Alcohol use disorder, or history of or
Brain problems (including tumors, increased intracranial pressure) or
Breathing problems (eg, asthma, apnea, low oxygen levels, sleep apnea) or
Chronic obstructive pulmonary disease (COPD) or
Cor pulmonale (serious heart condition) or
Gallbladder disease (eg, gallstones) or
Depression, history of or
Drug dependence, including opioid or illicit drug use disorder or dependence, history of or
Head injury, history of or
Mental health problems, history of or
Weakened physical condition—Use with caution. May increase risk for more serious side effects.
Asthma, acute or severe or
Respiratory depression (serious breathing problem) or
Short-term pain or
Stomach or bowel blockage (including paralytic ileus), known or suspected—Should not be used in patients with these conditions.
Bradyarrhythmia (slow heart rhythm) or
Hypotension (low blood pressure) or
Pancreatitis (swelling of the pancreas), acute or
Seizures, history of—Use with caution. May make these conditions worse.
Kidney disease or
Liver disease—Use with caution. The effects may be increased because of slower removal of the medicine from the body.
The fentanyl skin patch is only used for opioid-tolerant patients. A patient is opioid-tolerant if oral opioids have already been used for severe pain.
Taking 2 opioids together can increase the chance of serious side effects.
This medicine will add to the effects of alcohol and other CNS depressants. CNS depressants are medicines that slow down the nervous system, which may cause drowsiness or make you less alert. Some examples of CNS depressants are antihistamines or medicine for hay fever, other allergies, or colds, sedatives, tranquilizers, or sleeping medicine, other prescription pain medicine or opioids, benzodiazepines, medicine for seizures or barbiturates, muscle relaxants, or anesthetics, including some dental anesthetics.
Using too much fentanyl skin patch, or taking too much of another opioid with fentanyl skin patch, may cause an overdose.
Symptoms of an overdose include: drowsiness, extreme dizziness or weakness, irregular, fast or slow, or shallow breathing, pale or blue lips, fingernails, or skin, pinpoint pupils, relaxed and calm, slow heartbeat or breathing, seizures, sleepiness, trouble breathing, or cold, clammy skin.
This medicine may cause sleep-related breathing problems (eg, sleep apnea, sleep-related hypoxemia).
SIDE EFFECTS:
Anxiety
bloating or swelling of the face, arms, hands, lower legs, or feet
burning, crawling, itching, numbness, prickling, "pins and needles", or tingling feelings
confusion
decrease in urine volume
difficulty in breathing or swallowing
difficulty in passing urine (dribbling)
fast, irregular, pounding, or racing heartbeat or pulse
painful urination
rapid weight gain
seeing, hearing, or feeling things that are not there
skin itching, rash, or redness
swelling of the face, throat, or tongue
tremor
unusual weight gain or loss
upper stomach pain
Bluish color of the fingernails, lips, skin, palms, or nail beds
burning, itching, redness, skin rash, swelling, or soreness at the application site
confusion about identity, place, and time
false or unusual sense of well-being
irregular, fast or slow, or shallow breathing
Agitation
blurred vision
chest pain, discomfort, or tightness
cough
darkening of the skin
diarrhea
dizziness, faintness, or lightheadedness when getting up suddenly from a lying or sitting position
fever
headache
hives
lightheadedness, dizziness, or fainting
loss of appetite
mental depression
nausea
nervousness
overactive reflexes
poor coordination
pounding in the ears
restlessness
severe constipation
severe vomiting
shivering
sweating
talking or acting with excitement you cannot control
unusual tiredness or weakness
vomiting
Constipation
feeling cold
sleepiness or unusual drowsiness
trouble sleeping
Dry mouth
feeling of constant movement of self or surroundings
feeling of crawling, tingling, or burning of the skin
lack or loss of strength
memory loss
sensation of spinning
unusual dreams
Abnormal ejaculation
decreased interest in sexual intercourse
decreased sexual performance or desire
inability to have or keep an erection
loss in sexual ability, desire, drive, or performance
muscle twitching
Belching
heartburn
indigestion
stomach discomfort or upset
SOURCE:
Fentanyl (transdermal route) - Side effects & dosage - Mayo Clinic
Dr. Oz pledges to tackle hospice fraud: "Do not steal from the American people"
March 13, 2026:
Dr. Mehmet Oz pledged this week to lead an effort that would decertify any hospice providers that are found to be defrauding taxpayers by stealing the identities of people not in hospice or by overbilling for those who are dying.
"If they steal the money, they'll steal your health, they'll steal your life, and we're seeing that over and over again, which is why we have to send a very loud message to fraudsters that we're not open for business for you," said Oz, who is the Trump administration's administrator for the Centers for Medicare and Medicaid Services.
The hospice industry has in recent years suffered at the hands of bad actors who have billed the federal government for services they never provided, or for people who are not even sick.
Nationwide, the U.S. Department of Health and Human Services Office of the Inspector General reported in 2023 that suspected hospice fraud amounts totaled an estimated $198.1 million.
These people need to be held accountable for not only fraud, but for MURDER! Imagine how much hospice fraud/murder Michigan has with the guardianship problem that is running rampant in our corrupt probate court system to steal people’s lives and estates!
Read full story here:
Dr. Oz pledges to tackle hospice fraud: "Do not steal from the American people" - CBS News
“Comfort” Kit: Ativan (Lorazepam)
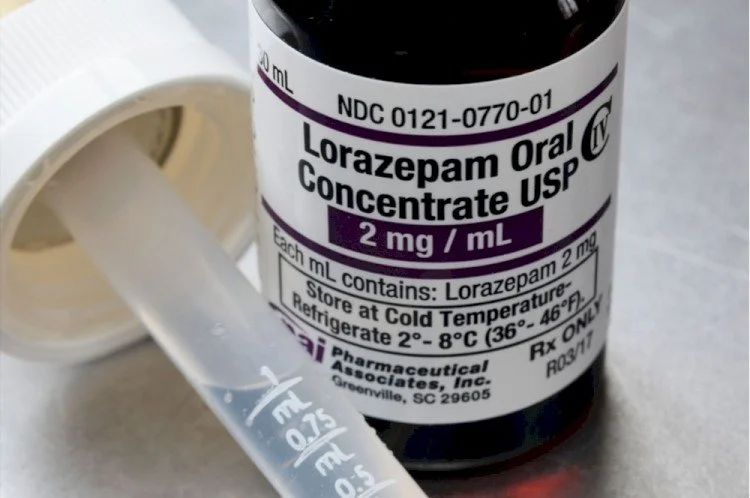
Commonly used Hospice drugs:
*Pain Management: Morphine (Roxanol), Hydrocodone, Dilaudid, Methadone, and Acetaminophen (suppository).
*Anxiety/Restlessness: Lorazepam (Ativan), Haloperidol (Haldol), Quetiapine, and Thorazine.
*Nausea/Vomiting: Haloperidol, Prochlorperazine (Compazine), Promethazine (Phenergan), and Reglan.
*Respiratory Distress/Excess Secretions: Atropine (drops), Hyoscyamine (Levsin), and Morphine.
*Constipation/Other: Bisacodyl (Dulcolax) and other stool softeners. Benadryl.
***RISKS***
Mixing benzodiazepines (Ativan) with opioids (Morphine) or antipsychotics (Haldol) causes falls, confusion, respiratory depression, coma/sedation, and death especially in older adults.
ATIVAN (LORAZEPAM)
Lorazepam is used to treat anxiety disorders. Lorazepam is a benzodiazepine that works in the brain to relieve symptoms of anxiety. Benzodiazepines are central nervous system (CNS) depressants, which are medicines that slow down the nervous system.
Elderly patients are more likely to have unwanted effects (eg, severe drowsiness or unsteadiness) and age-related kidney, liver, or heart problems, which may require caution and an adjustment in the dose.
Symptoms of an overdose include: blurred vision, change in consciousness, confusion, dizziness, faintness, or lightheadedness when getting up suddenly from a lying or sitting position, hallucinations, increased sweating, loss of consciousness, loss of strength or energy, muscle pain or weakness, nightmares, shakiness and unsteady walk, slow or irregular heartbeat, sweating, trouble in speaking, unsteadiness, trembling, or other problems with muscle control or coordination, trouble sleeping, unusual excitement, nervousness, restlessness, or irritability, or unusual tiredness or weakness.
This medicine may cause respiratory depression (serious breathing problem that can be life-threatening), especially when used with narcotic pain medicines.
This medicine will add to the effects of alcohol and other central nervous system (CNS) depressants. CNS depressants are medicines that slow down the nervous system, which may cause drowsiness or make you less alert. Some examples of CNS depressants are antihistamines or medicine for hay fever, allergies, or colds, sedatives, tranquilizers, or sleeping medicine, prescription pain medicine or narcotics, barbiturates or medicine for seizures, muscle relaxants, or anesthetics (numbing medicines), including some dental anesthetics.
***SIDE EFFECTS***
Drowsiness
relaxed and calm
sleepiness
Aggressive, angry
agitation
attack, assault, or force
black, tarry stools
bleeding gums
blood in the urine or stools
bluish lips or skin
blurred vision
change in consciousness
chest tightness
chills
coma
confusion
confusion about identity, place, and time
cough or hoarseness
dark urine
decreased urine output
difficulty with breathing or swallowing
difficulty with speaking
discouragement
dizziness, faintness, or lightheadedness when getting up suddenly from a lying or sitting position
drooling
dry mouth
excitation
false or unusual sense of well-being
fast or irregular heartbeat
feeling sad or empty
fever with or without chills
general feeling of tiredness or weakness
headache
hives, itching, or rash
hyperventilation
increased thirst
irregular, fast or slow, or shallow breathing
irritability
loss of appetite
loss of balance control
loss of consciousness
loss of interest or pleasure
loss of memory
lower back or side pain
muscle pain, cramps, trembling, jerking, or stiffness
nausea or vomiting
not breathing
painful or difficult urination
pale or blue lips, fingernails, or skin
pinpoint red spots on the skin
problems with memory
puffiness or swelling of the eyelids or around the eyes, face, lips, or tongue
reddening of the skin, especially around ears
restlessness
seeing, hearing, or feeling things that are not there
seizures
shaking
shuffling walk
sore throat
sores, ulcers, or white spots on the lips or in the mouth
stiffness of the limbs
stomach pain
sweating
swelling of the eyes or inside of the nose
swelling of the face, ankles, or hands
swollen glands
thoughts or attempts at killing oneself
trouble concentrating
trouble sleeping
twisting movements of body
uncontrolled movements, especially of the face, neck, and back
unexplained bleeding or bruising
unpleasant breath odor
unusual bleeding or bruising
unusual tiredness or weakness
vomiting of blood
yellow eyes or skin
Being forgetful
clumsiness
constipation
decreased interest in sexual intercourse
disturbed color perception
dizziness or lightheadedness
double vision
drowsiness
feeling of constant movement of self or surroundings
hair loss or thinning of the hair
halos around lights
inability to have or keep an erection
increased in sexual ability, desire, drive, or performance
increased interest in sexual intercourse
lack or loss of self-control
lethargy
loss in sexual ability, desire, drive, or performance
muscle aches, twitching, or weakness
night blindness
overbright appearance of lights
rapid weight gain
sensation of spinning
shakiness in the legs, arms, hands, or feet
shivering
stupor
trembling or shaking of the hands or feet
tunnel vision
weak or feeble pulse
SOURCE:
Lorazepam (oral route) - Side effects & dosage - Mayo Clinic
WOMAN GETS PRISON FOR PRETENDING TO BE A NURSE
Leticia Gallarzo, 51, who used to live in Wayland, Michigan, was sentenced on Monday, January 26, 2026 to 6 years, 3 months in prison for identity theft and falsifying medical records saying she was licensed as a registered nurse and for pretending to be a real nurse licensed in Michigan, according to the United States Attorney’s Office.
She used the fake nursing license to work at a West Michigan health facility (nursing home). She pleaded guilty to the federal charges in November of 2023, but then skipped sentencing scheduled for July 2024.
She worked as a (fake) registered nurse from August 2022 to May 2023 at a Grand Rapids hospice care facility. She got the job through Indeed.com by pretending to be an actual registered nurse and provided a fake nursing license, diploma, and identification documents to make it look like she had been trained as a nurse.
After she got that job, she was promoted to unit manager, meaning she supervised other health care professionals in the care they provided to the nursing home residents. During her time at the facility, she conducted patient assessments, administered medications, started intravenous lines, and cared out other nurses’ duties. Eventually, her “performance as a nurse faltered,” attorneys said, and she was demoted. As she applied to other jobs, a prospective employer figured out she was not who she said she was and reported her.
After she was charged, plead guilty, and skipped sentencing, she fled to Illinois and then California, where she got jobs as a physician assistant and registered nurse. She was found in Los Angeles and brought back to Michigan for Monday’s sentencing.
She has a pattern of this and has been convicted before. In 2016, she was convicted of impersonating a licensed nurse in Kent County and convicted of the same thing in Texas in 2017.
U.S. Attorney VerHey said, “This is far more than a fraud case. Nurses make life and death decisions for the people under their care, and everyone has a right to expect that their health is being attended by a person with extensive medical training.”
“This 75-month federal prison sentence sends a clear and unmistakable message: no one gets to lie about their credentials, falsify medical records, or steal identities without facing serious consequences,” Jennifer Runyan, Special Agent in Charge of the FBI Detroit Field Office, said in a statement. Leticia Gallarzo abused the trust placed in medical professionals and put patients at risk. Because of the relentless work of the FBI Grand Rapids Resident Agency, she can no longer fraudulently perform patient assessments or endanger the community.”
The Federal Bureau of Investigation, Detroit Division, Grand Rapids Field Office investigated this case. Assistant U.S. Attorney Ron Stella prosecuted the case.
SOURCES:
‘More than a fraud case’: Woman gets prison for pretending to be nurse | WOODTV.com

“Comfort” Kit: Morphine (Roxanol)
Commonly used Hospice drugs:
*Pain Management: Morphine (Roxanol), Hydrocodone, Dilaudid, Methadone, and Acetaminophen (suppository).
*Anxiety/Restlessness: Lorazepam (Ativan), Haloperidol (Haldol), Quetiapine, and Thorazine.
*Nausea/Vomiting: Haloperidol, Prochlorperazine (Compazine), Promethazine (Phenergan), and Reglan.
*Respiratory Distress/Excess Secretions: Atropine (drops), Hyoscyamine (Levsin), and Morphine.
*Constipation/Other: Bisacodyl (Dulcolax) and other stool softeners. Benadryl.
***RISKS***
Mixing benzodiazepines (Ativan) with opioids (Morphine) or antipsychotics (Haldol) causes falls, confusion, respiratory depression, coma/sedation, and death especially in older adults.
MORPHINE (ROXANOL)
Morphine is used to treat pain severe enough to require daily, around-the-clock, long-term opioid treatment and when other pain medicines did not work well enough or cannot be tolerated. Morphine belongs to the group of medicines called narcotic analgesics (pain medicines). It acts on the central nervous system (CNS) to relieve pain. CNS depressants are medicines that slow down the nervous system, which may cause drowsiness or make you less alert.
Roxanol is an oral solution of Morphine. The recommended dose for adults according to Mayo Clinic is 10-20 milligrams every 4 hours as needed for moderate to severe pain, but in Hospice they typically give this medication (along with a benzo or other drugs) every 2 hours or less.
This medicine may cause sleep-related breathing problems (eg, sleep apnea, sleep-related hypoxemia).
This medicine will add to the effects of other central nervous system (CNS) depressants. Some examples of CNS depressants are antihistamines or medicine for allergies or colds, sedatives, tranquilizers, or sleeping medicine, other prescription pain medicine or narcotics, medicine for seizures or barbiturates, muscle relaxants, or anesthetics, including some dental anesthetics.
***SIDE EFFECTS***
Blurred vision
bulging soft spot on the head of an infant
burning, crawling, itching, numbness, prickling, "pins and needles", or tingling feelings
change in the ability to see colors, especially blue or yellow
chest pain or discomfort
chills
confusion
cough
decreased urination
dizziness, faintness, or lightheadedness when getting up suddenly from a lying or sitting position
fainting
fast, pounding, or irregular heartbeat or pulse
headache
hives, itching, or skin rash
increased sweating
loss of appetite
nausea
nervousness
pounding in the ears
puffiness or swelling of the eyelids or around the eyes, face, lips, or tongue
severe constipation
severe vomiting
shakiness in the legs, arms, hands, or feet
slow heartbeat
stomach pain
sweating
vomiting
Agitation
black, tarry stools
chest tightness
cold, clammy skin
darkening of the skin
diarrhea
difficulty swallowing
feeling of warmth or heat
fever
flushing or redness of the skin, especially on the face and neck
increased sensitivity to pain
irregular, fast or slow, or shallow breathing
lightheadedness
loss of consciousness
low blood pressure or pulse
mental depression
overactive reflexes
painful urination
pale or blue lips, fingernails, or skin
pale skin
pinpoint red spots on the skin
poor coordination
pounding in the ears
puffiness or swelling of the eyelids or around the eyes, face, lips, or tongue
restlessness
shakiness and unsteady walk
shivering
talking or acting with excitement you cannot control
twitching
unsteadiness, trembling, or other problems with muscle control or coordination
unusual bleeding or bruising
unusual tiredness or weakness
very slow heartbeat
worsening of pain
Cramps
difficulty having a bowel movement
drowsiness
false or unusual sense of well-being
relaxed and calm feeling
sleepiness or unusual drowsiness
weight loss
Absent, missed, or irregular menstrual periods
bad, unusual, or unpleasant (after) taste
change in vision
dry mouth
floating feeling
halos around lights
heartburn or indigestion
loss in sexual ability, desire, drive, or performance
muscle stiffness or tightness
night blindness
overbright appearance of lights
problems with muscle control
stomach discomfort or upset
trouble sleeping
uncontrolled eye movements
Abnormal dreams
change in walking and balance
change or problem with discharge of semen
clumsiness or unsteadiness
confusion as to time, place, or person
false beliefs that cannot be changed by facts
feeling of constant movement of self or surroundings
general feeling of discomfort or illness
holding false beliefs that cannot be changed by fact
poor insight and judgment
problems with memory or speech
seeing, hearing, or feeling things that are not there
sensation of spinning
trouble recognizing objects
trouble thinking and planning
trouble walking
unusual excitement, nervousness, or restlessness
***Symptoms of overdose***
Constricted, pinpoint, or small pupils (black part of the eye)
decreased awareness or responsiveness
extreme drowsiness
fever
increased blood pressure
increased thirst
lower back or side pain
muscle cramps, spasms, pain, or stiffness
no muscle tone or movement
severe sleepiness
swelling of the face, fingers, or lower legs
weight gain
SOURCE:
Sixteen Charged in Detroit Area as Part of Largest National Medicare Fraud Takedown in History
On June 18, 2015, Attorney General Loretta E. Lynch and Department of Health and Human Services (HHS) Secretary Sylvia Mathews Burwell announced a nationwide sweep let by the Medicare Fraud Strike Force in 17 districts, resulting in charges against 243 individuals including 46 doctors, nurses, and other licensed medical professionals, for their alleged participation in Medicare fraud schemes involving approximately $712 million in false billings.
In the Detroit area, sixteen individuals, including six doctors, a social worker, a pharmacist, and two physical therapists were charged with a variety of health care fraud and kickback schemes totaling over $122 million. The schemes involved services that were medically unnecessary or never rendered, including physician visits, hospice care, home health care, and the billing but not dispensing of pharmaceuticals.
The following charges were filed or unsealed:
United States v. Tahir, et al.
Five individuals, two physicians and three owners of hospice and home health care companies, were charged in an indictment and conspiring to commit health care fraud for their roles in a $58.3 million scheme to defraud Medicare by submitting fraudulent claims for home health care and hospice services that were medically unnecessary or not provided. The owners of the home health care and hospice companies, two of whom are also physical therapists, paid physicians and recruiters kickbacks for referring patients, then billed Medicare for medically unnecessary services, which were often never provided. The companies, located in Livonia, Michigan, are A Plus Hospice and Palliative Care, At Home Hospice, and At Home Network Inc., a home health care agency. The physicians who solicited and received kickbacks also submitted claims to Medicare for medically unnecessary physician services through their companies, Waseem Alam, M.D., P.C., Woodward Urgent Care, and Hatem Ataya, M.D., P.C. Those physicians prescribed beneficiaries medically unnecessary prescriptions, including controlled substances, for which Medicare also paid.
The defendants charged in the indictment are Shahid Tahir, 45, of Bloomfield, Michigan, Waseem Alam, 59, of Troy, Michigan, Hatem Ataya, 47, of Flushing, Michigan, Muhammad Tariq, 60, of West Bloomfield, Michigan, Manawar Javed, 40, of West Bloomfield, Michigan.
Read the whole story:
Sixteen Charged in Detroit Area as Part of Largest National Medicare Fraud Takedown in History — FBI

